What Is a Pleurectomy/Decortication?
A pleurectomy/decortication is a two-part surgical procedure used in the treatment of malignant pleural mesothelioma.
- Pleurectomy removes part or all of the pleura (the thin membrane surrounding the lungs).
- Decortication removes visible mesothelioma tumors from the chest cavity.
Pleurectomy with decortication surgery is an effective way to control the spread of pleural mesothelioma while relieving shortness of breath, chest pain, and other symptoms.
Getting a pleurectomy/decortication for mesothelioma can increase your life expectancy and improve your quality of life. P/D also comes with shorter recovery times and fewer side effects than extrapleural pneumonectomy (EPP), another type of surgery for pleural mesothelioma that completely removes the affected lung.
This surgical approach was pioneered in the 1990s by thoracic surgeon Dr. Robert Cameron as a lung-sparing option for patients with mesothelioma cancer.
Mesothelioma Hope has relationships with highly trained surgeons who can determine if P/D surgery is an option for you or a loved one.
Who’s Eligible for a Pleurectomy With Decortication?
P/D is generally offered to patients with early-stage pleural mesothelioma (stages 1 and 2). This means their cancer is limited to the chest cavity and hasn’t spread to other areas of the body.
By the third and fourth stages of mesothelioma, tumors may have spread too far to be effectively removed through P/D surgery.
According to Baylor College of Medicine, P/D is commonly preferred to EPP, especially for patients who can’t undergo total mesothelioma lung removal.
Pleural mesothelioma patients must be in good overall health to undergo a P/D so their body can fully recover. Doctors will usually order blood work, pulmonary function tests (lung function tests), and an echocardiogram (heart ultrasound) to determine if a patient is healthy enough for a P/D.
What Is Pleurectomy Surgery?
Pleurectomy surgery is the first part of a mesothelioma pleurectomy with decortication. This is when the surgeon removes the lining of the lungs, called the pleura.
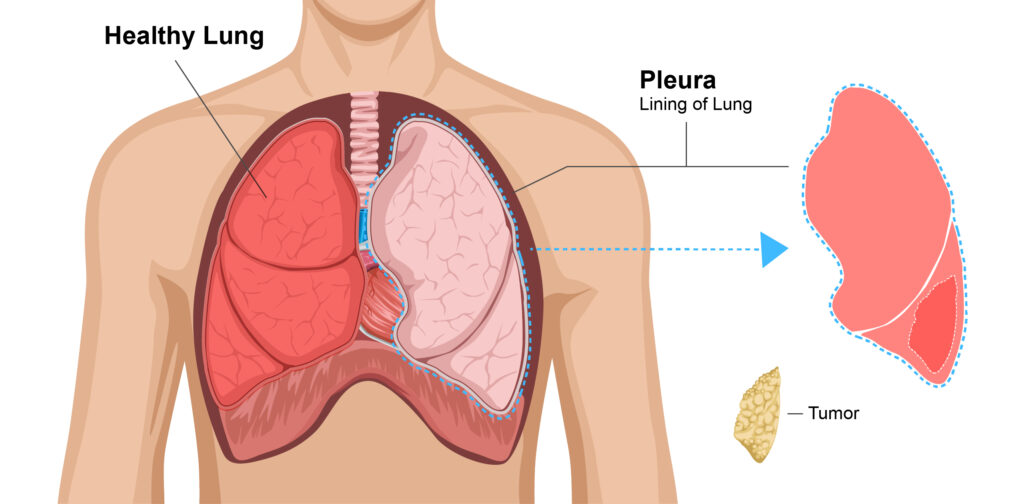
During the pleurectomy procedure:
- A surgeon places the patient on their side and makes an S-shaped incision (cut) along the patient’s back.
- The surgeon removes part or all the pleura, depending on the extent of the cancer.
- The surgeon may also remove parts of the chest wall lining, heart lining (pericardium), diaphragm, or lymph nodes if they find tumors in these areas. This is known as an extended pleurectomy with decortication (EPD).
The surgeon may also need to remove the patient’s sixth rib in order to access the entire pleural space. Once the pleura and any other cancerous tissues have been carefully removed, the decortication procedure can begin.

“Instead of removing the lung, you carefully separate the tumor from the healthy lung.”
What Is Decortication of the Lung?
Decortication is the second part of a pleurectomy/decortication for mesothelioma. During this surgery, visible tumors are removed from the surface of the lung and the rest of the chest to reduce the risk of the cancer coming back.
During the decortication procedure:
- The surgeon uses a scalpel to remove visible tumor growth in the chest cavity.
- Specialists then pack the area with hot gauze and sponge packs to limit blood loss.
- Once the bleeding has slowed, the surgeon uses sutures (stitches) to close the incision.
Doctors will schedule follow-up appointments after the surgery to see how the patient is recovering and see if there have been any complications.
P/D With HITHOC
Similar to EPP, P/D surgery is often paired with hyperthermic intrathoracic chemotherapy (HITHOC). A heated chemotherapy solution is administered to the chest cavity right after the operation to kill any remaining cancer cells before the patient’s incision is closed.
Pleurectomy/Decortication Recovery Time
Total recovery time from a P/D is usually 4-6 weeks if part of the pleura is removed, and 6-8 weeks if the entire pleura is removed.
After surgery, patients will be put on a respirator to help them breathe. When the patient can breathe on their own, chest tubes are fitted to help inflate their lungs and drain any fluid buildup (pleural effusion). Most patients spend 7-10 days in the hospital before being discharged.
Caregivers may need to monitor their loved one once they’re back home to make sure they’re comfortable and recovering well. During this time, the patient’s doctor may recommend at-home breathing exercises to improve lung function.
If you or a loved one is exploring treatment options for pleural mesothelioma, our Free Doctor Checklist can help you prepare for your next appointment.
What Is the Success Rate of Pleurectomy and Decortication?
A pleurectomy/decortication has shown to double the life expectancy of patients with pleural mesothelioma.
Specifically, patients who receive a mesothelioma pleurectomy with decortication live for 34 months on average, almost twice as long as the average life expectancy of pleural mesothelioma.
P/D surgery also has a positive impact on survival rates (the percentage of people who survive mesothelioma for a specific amount of time). According to a report in the Journal of Thoracic Disease, 60.9% of patients are still alive 2 years after the procedure, and 29.2% live at least 5 years.
Interestingly, the MARS 2 clinical trial found that extended P/D surgery was less effective than chemotherapy and resulted in more complications, according to a June 2024 report in The Lancet Respiratory Medicine.
Pleurectomy/Decortication Side Effects
Potential side effects of P/D mesothelioma surgery include:
- Air leaks (when small pockets of air escape the lungs)
- Internal bleeding or blood clots
- Irregular heartbeat (arrhythmia)
- Lung or heart failure
- Pneumonia and other infections
- Reactions to general anesthesia
Patients should discuss all potential side effects with their mesothelioma doctor before deciding to undergo a pleurectomy with decortication.
Find Doctors for Pleurectomy/Decortication Surgery
If you or a loved one has been diagnosed with early-stage pleural mesothelioma, a pleurectomy with decortication can be an effective procedure to help you live longer and breathe more easily.
Mesothelioma Hope can help you explore your treatment options and connect you with doctors who are experienced in pleurectomy/decortication surgery.
Call us now at (866) 608-8933 or use our Free Doctor Match to find pleural mesothelioma specialists in your area.
Mesothelioma Hope has no affiliation with and is not endorsed or sponsored by Dr. Robert Cameron. Any contact information listed is for informational purposes only. You have the right to contact Dr. Robert Cameron directly.
Mesothelioma Pleurectomy With Decortication FAQs
What is a pleurectomy decortication for mesothelioma?
A pleurectomy/decortication (P/D) is a surgery used to treat pleural mesothelioma, which affects the lining around the lungs. In this surgery, doctors remove the cancer-affected lining of the lung (the pleura) and any thick tumor or scar tissue that is pressing on the lung.
The goal is to remove as much cancer as possible while keeping the lung in place. This can help patients breathe easier, reduce symptoms, and improve quality of life.
Is decortication the same as pleurectomy?
No, pleurectomy and decortication are not the same, but they are often done together to treat pleural mesothelioma. A pleurectomy removes the cancer-affected lining around the lungs. Decortication removes a thick layer of tumor or scar tissue that can keep the lung from expanding. Doing both can help patients breathe easier and keep as much lung function as possible.
Is a pleurectomy major surgery?
Yes, a pleurectomy is major surgery. You’ll receive general anesthesia before the procedure and spend about 7-10 days in the hospital afterward being monitored by your health care team.
Despite a pleurectomy being an invasive surgical treatment, it’s been shown to extend overall survival, improve lung function, and offer a better quality of life for patients diagnosed with pleural mesothelioma.
How long does a pleurectomy take?
The pleurectomy portion of pleurectomy/decortication surgery takes roughly 1-2 hours.
Exactly how long it’ll take in your case depends on whether the surgeon needs to take out parts of the chest wall lining or diaphragm along with the pleura (lung lining), or if any postoperative complications occur.






