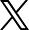Following a milestone birthday celebration, a mother’s visit to a gynecologist leads to the discovery of a mysterious illness that baffled her doctors
Since being diagnosed with mesothelioma in 2009, Jill Litton has noticed a recurring theme throughout her health care journey: confusion. But she has met that confusion with grace and faith as she continues in her decade-and-a-half fight against this rare cancer.
“I don’t accept death,” says the West Virginia native, with genuine seriousness behind her soft laughter and calm voice. “My family needs me, and I have to keep living my best so I can take care of them.”
She attributes her survival to her unwavering faith in God’s plan for her life and her belief she would somehow manage to survive.
Confusing Symptoms Lead to a Mesothelioma Diagnosis
After celebrating her 50th birthday, Jill experienced a prolonged menstrual cycle that lasted several weeks rather than a few days.
Confiding in a handful of coworkers, the mother of two was assured that the symptoms she was experiencing were caused by “the change” — a euphemism referring to her transition into menopause. Besides some discomfort, she experienced few other symptoms.
During a gynecological exam the following month, Jill was told she was hemorrhaging and required emergency care. Three exploratory incisions showed an unidentified grayish-white substance covering her reproductive organs. A biopsy confirmed it was peritoneal mesothelioma, a type of this cancer that develops in the abdominal lining.

“I didn’t even know what mesothelioma was. The medical staff didn’t know how to handle it, either. They kept saying that my test results were so unusual that they must be wrong.”
The following days were hazy with questions and tests, resulting in a hysterectomy. Although her family’s medical history includes various cancers, mesothelioma was unfamiliar territory. “No one believed me,” she recalls. “Even when new tests confirmed that I have peritoneal mesothelioma, doctors were again confused.”
Jill’s mesothelioma diagnosis, particularly the way it presented on her reproductive organs, continues to bewilder her doctors and care team. They remind her how unusual it has been to witness.
Many other survivors like Jill have shared how confusing or shocking their diagnosis was. Read their stories in our Free Mesothelioma Survivors Guide.
Tracking Down Her Source of Asbestos Exposure
The question of how Jill was exposed to asbestos — the only known cause of mesothelioma — confused all her doctors, nurses, and lab technicians.
Perhaps the biggest piece of this puzzle is her late father, who served in the United States Navy for seven years. Jill suspects her father’s daily exposure to asbestos — large amounts of which were often found on his clothes — may offer an explanation.
Since asbestos is durable and affordable — and because manufacturers of asbestos-containing products hid the dangers of the mineral for decades — it was frequently used in materials for constructing military equipment and buildings.
This continued exposure to asbestos put millions of innocent people at risk of developing mesothelioma. In fact, because the U.S. military relied on asbestos products for much of the 20th century, veterans now make up about 33% of all mesothelioma cases.
As a child, Jill played on the same floor where asbestos dust from her father’s work clothes landed each night. She may have ingested asbestos for years without knowing.
Our team of compassionate Patient Advocates can help you track down where and how you or a loved one were exposed to asbestos, even if you don’t remember. Call (866) 608-8933 now to get the answers you need.
Letting Go and Finding Peace
Jill’s diagnosis was deeply heartbreaking for her mother, who blamed herself for the potential negligence that led to her daughter’s illness. Jill, however, doesn’t hold any of her family members responsible for her diagnosis.
“I always reminded her that it was silly to feel guilty because I could have been exposed to asbestos anywhere,” Jill says.
Despite what may have happened in her life that led to this diagnosis, Jill doesn’t hold any feelings of resentment or anger toward her loved ones.







“I don’t feel bad about having mesothelioma. I have never felt sorry for myself. Worse things have happened to other people. This is something that I will never totally understand, and that’s okay.”
Heaven Knows How Treatment Will Go
Many of Jill’s existing doctors were unfamiliar with mesothelioma treatment. She was told there might not be much they could do for her.
Jill refused to accept this news and started looking for a mesothelioma specialist. Once she found the right doctor, she was able to get cytoreductive surgery with heated chemotherapy (HIPEC) to remove her tumors and kill any cancer cells left behind.







“Just because you have cancer and your doctor says you have a year to live doesn’t mean you must suddenly agree to those terms and begin preparing to die.”
Patients with peritoneal mesothelioma who undergo cytoreductive surgery with HIPEC have an average life expectancy of 53 months.
Jill has lived nearly four times longer than what survival statistics project, a fact she connects to her strong faith.
“Most doctors tell you that you only have a year to live. From the moment I heard those words at the hospital, I completely trusted God with my whole heart,” says Jill. “He has continually blessed me, and I am still here more than a decade later.”
Calling on Faith to Overcome Treatment Challenges
Recalling the various mesothelioma treatment options she has pursued, Jill reveals that the only time she questions her faith is during her regular chemotherapy appointments, which are spaced three weeks apart.
For a week following chemotherapy, Jill experiences such intense nausea that she must stay at the hospital for several days to receive 24/7 medical care. By the second week, she usually feels strong enough to continue recovering at home before her next session.
“Chemotherapy takes such an extreme toll on my body that even my doctor told me he has never seen anyone react this badly to it,” she shares.







“Each time I go through chemotherapy, I ask God why it has to be this hard on me. But then I realize that I would rather vomit for several weeks in exchange for remaining alive for another several years.”
Survivor’s guilt is another area of emotional, social, and spiritual struggle for Jill.
“I have lost people who should have outlived me, and I went to their funerals,” she says. “Sometimes I cry and wonder why another mom died when she had a young daughter or son to raise.”







“As much as I am thankful that I am still alive, I also struggle with extreme guilt because not everyone is this lucky.”
Learn more about how survivors managed mesothelioma treatment in our Free Mesothelioma Survivors Guide.
Finding Strength in Caring for Others
After a series of traumatic events drastically altered the course of her older son’s life, Jill stepped in to help raise his two children.
Her now teenage and pre-teen granddaughters, both of whom are fully aware of her diagnosis, have been homeschooled under her supervision.
“Although their story is sad, and I have cried a million tears over it, it’s also a gift from God that I get to nurture them. I don’t know how their story will end, but I know it will be great,” Jill reveals.
“They have watched me suffer tremendously, and they are so kind, loving, and helpful to me. I can’t wait to see what good things are in store for them.”
When her granddaughters were babies, Jill was worried that the weakness and pain she experienced from her chemotherapy sessions would prevent her from properly caring for them.
However, she soon discovered that caring for these girls gave her the motivation, emotional support, and strength she needed to get out of bed every morning and continue living her life as normally as possible.
Now, Jill believes that raising her granddaughters is a huge part of her will to survive.







“These children have given me the courage and determination to continue fighting. My life is absolutely wonderful. What more could I ask for?”
Get Help Fighting Mesothelioma
A mesothelioma diagnosis can be emotionally and physically draining for patients and their families. If you or someone you love is suffering from this devastating cancer, you don’t have to take this journey alone.
Mesothelioma Hope’s caring team of Patient Advocates is ready to provide personalized medical, financial, and supportive care to ease your stress and inspire hope.
Call us at (866) 608-8933 now for help, or get a Free Survivors Guide to read more stories of resilience directly from mesothelioma patients.